Items filtered by date: June 2024
Benefits of Practicing Yoga
 A routine yoga practice can reel in benefits like:
A routine yoga practice can reel in benefits like:
- Increased endurance, flexibility & muscle strength
- Improved core strength, athletic performance & balance
- Injury prevention
- Mental relaxation & focus, and more!
There IS something for everyone... from simple stretches to advanced power poses.
Got a desk job? Focus on your posture with seated twists, shoulder rolls, wide-leg forward bend, seated figure 4 stretch, seated backbend stretch, seated crescent moon, stork pose, wrist rolls. Or start with this video.
Commute much? Try these seat-friendly stretches when you're at your destination: Seated mountain pose, seated cat/cow pose, seated cobra pose, seated spinal twist, neck rolls, seated forward fold, and anterior shoulder stretch.
Need more cardio? Try power yoga vinyasas that include chaturanga dandasana, warrior poses, and arm-balancing poses.
Constantly stressed? Check out restorative yoga and use props to help you relax, clear your mind, and decompress.
Not sure what's right for you? Learn more about different yoga practices here.
Tips for beginners:
- Breath. Pay attention to your breath and breathe deeply. Fill up your lungs! Inhale when opening the front of the body, and exhale when compressing the front of the body. (Or follow your instructor!)
- Slow down. Focus on intentional movement.
- Listen to your body. Make modifications if something doesn't feel right. Start with beginner poses and work your way up to advanced.
Get started today and feel the benefits of yoga for yourself!
Foot Cramps 101
 What are they?
What are they?
Foot cramps are a common, involuntary muscle spasm with a sharp or deep aching sensation, lasting seconds, minutes, or even days. Common causes include:
- Dehydration
- Overuse/ overexertion
- Prolonged sitting or standing
- Pregnancy
- Tight footwear
- Electrolyte imbalances/ poor diet
How to manage:
- Apply heat to increase blood flow, improve flexibility and relax muscles.
- Stretch slowly to help alleviate symptoms.
- Massage the affected area to increase blood flow and decrease lactic acid buildup.
- Wear supportive shoes that are properly sized with space to wiggle toes.
- Stay hydrated! Drink water throughout the day.
- Eat a healthy, balanced diet to provide adequate vitamins, minerals, and nutrients to your body.
Foot cramps may also be a sign of nerve damage or an underlying health condition. Some medications have side effect profiles that include cramping. Talk to your healthcare provider if your foot cramps aren't improving.
Surprising causes of leg cramps
 Leg cramps are more common than you think. Some reasons you may be familiar with, but others might surprise you:
Leg cramps are more common than you think. Some reasons you may be familiar with, but others might surprise you:
- your weight
- dehydration/ low levels of electrolytes
- lack of blood flow
- nerve compression
- pregnancy
- under-training / overexertion
- medications (diuretics, NSAIDs, statins, birth control pills, and more)
- medical conditions involving your kidneys, thyroid, liver, circulation, and more
Suggestions for prevention:
- Check your weight. If you're over a healthy weight and need help putting together a weight-loss plan or diet, talk to your doctor. We're here to help!
- Drink enough water. Check out my blog post on personalized water consumption: https://www.ezfootankle.com/post/you-are-what-you-drink
- Warm up with dynamic movements and stretching before exercise. Heat can be applied during/after cramping episodes to help increase blood flow and relax the muscle while stretching.
- Focus on proper training, form, and getting adequate rest. Muscle imbalances can also cause cramps, so be sure your training regimen is balanced (agonist/antagonist, eccentric/concentric, etc.)
- Replace electrolytes! Replenish through foods like low-fat yogurt, bananas, spinach, and lentils. Increase your intake of vitamin D, B (1 & 12), magnesium, zinc, and potassium. Sports drinks (low sugar options!) and supplement powder forms are convenient options.
To treat:
- Stop the movement that triggered the cramp
- Apply heat + gently stretch or massage the area
- Hydrate and replace electrolytes. (Pickle juice can work in a pinch!)
- Once the cramping episode subsides, continue to work on stretching and massaging that area over the next 24 hours.
- Work on prevention tips above!
If you're taking any medications that increase the risk of muscle spasms or cramps, talk to your doctor about options including switching to a different medication, changing your dose schedule, or re-evaluating its necessity. If you're experiencing cramping that persists despite lifestyle changes, or start to experience muscle weakness, skin color changes, leg swelling, increase in frequency of cramps, or severe pain, it may be a sign of something more serious and you should seek medical care immediately.
Back pain: How shoes affect your Spine
 The normal curvature of your spine functions to dissipate ground reactive forces (Newton's 3rd law #biomechanics). If your center of gravity changes due to an abnormal gait pattern, inadequate support, or lack of shock absorption, the spine can no longer disperse forces effectively, and your spinal curvature adapts. This adaptation, or malalignment, causes back pain.
The normal curvature of your spine functions to dissipate ground reactive forces (Newton's 3rd law #biomechanics). If your center of gravity changes due to an abnormal gait pattern, inadequate support, or lack of shock absorption, the spine can no longer disperse forces effectively, and your spinal curvature adapts. This adaptation, or malalignment, causes back pain.
Your center of gravity shifts as you walk from heel to toe, evenly distributing your weight through the feet. Normal walking mechanics are achieved with footwear that supports your body weight. Without proper support, your center of gravity is thrown off, causing an abnormal gait, leading to stress and strain up the kinetic chain (from your feet up to the spine). Good posture and proper alignment & support keeps the body happy and pain-free.
Final thoughts:
- Shoes should contain a shock absorptive material to help disperse forces from the ground as you walk, run, jump, or participate in activities. Many thin, flimsy flip flops don't provide this layer of protection, which is why you may experience pain after hours of wearing this type of unsupportive shoe. If you wouldn't want to wear the shoes to walk a mile, you probably shouldn't be wearing them at all!
- High heels change our center of gravity, increasing our spinal curvature (hyperlordotic lumbar spine) causing back pain. When you feel it's absolutely necessary to wear heels, limit your heel height to 1-2 inches and always bring a pair of comfortable shoes to change into.
- Flat shoes (ballet flats, flip flops, etc.) lack proper support, shock absorption, and also require your toes to flex or pinch to keep them on your feet. This shortens your stride, affects your center of gravity, again leading to back pain.
Your feet are your foundation. Your shoes affect more than just your feet they impact your ankles, knees, hips, and spine. If you experience back pain, the first place to look is down!
Do I need custom foot orthotics?
 Most people can benefit from custom foot orthotics, but whether you NEED them can be discussed with your doctor. A foot & ankle specialist will examine your feet and evaluate your biomechanics and foot function. Your foot structure, weight, activity level, medical conditions, and foot deformities/ areas of pain (bunion, hammertoe, callus, pinched nerve, heel spur, etc.) all play a role in determining your need for custom orthotics.
Most people can benefit from custom foot orthotics, but whether you NEED them can be discussed with your doctor. A foot & ankle specialist will examine your feet and evaluate your biomechanics and foot function. Your foot structure, weight, activity level, medical conditions, and foot deformities/ areas of pain (bunion, hammertoe, callus, pinched nerve, heel spur, etc.) all play a role in determining your need for custom orthotics.
What options do I have?
1. Over-the-counter (OTC) orthotics might be a solution for some. Well-made brands can offer support and cushioning, but they're "one-size-fits-all" and won't provide personalized correction. While less expensive, they will need to be replaced more often. Ask your doctor if they're an option for you, and if so, what style they recommend.
2. Custom foot orthotics are recommended when your feet need extra help to function properly. Conditions like flat feet or high arches are common examples. Without support, your muscles, tendons and ligaments work harder to absorb the shock of your body weight. Over time, lax ligaments and instability contribute to conditions like arthritis.
If you experience foot pain, discomfort, or fatigue, it's time to schedule an appointment with a foot & ankle specialist. Custom orthotics may be the solution you've been looking for.
Common causes of heel pain
 Heel pain can significantly impact daily activities and mobility, making it essential to identify the cause and seek appropriate treatment.
Heel pain can significantly impact daily activities and mobility, making it essential to identify the cause and seek appropriate treatment.
Heel pain presents as a symptom of many conditions, and it's crucial to identify the underlying cause before starting any treatment.
Common causes of heel pain:
- Achilles tendinitis
- Bone contusion
- Bursitis
- Fat pad atrophy
- Growth plate injuries
- Haglund's deformity/ pump bump
- Infection
- Inflammatory arthritis (gout, rheumatoid arthritis, ankylosing spondylitis, spondyloarthropathies)
- Nerve entrapment
- Osteoarthritis
- Peripheral Neuropathy
- Plantar fasciitis
- Plantar fibromatosis
- Posterior impingement
- Stress fractures
- Tumors or growths
When to seek treatment
If you experience persistent or severe heel pain, or discomfort that is affecting your daily life and ability to stay active, it's time to see a foot & ankle specialist. A thorough evaluation, physical exam, imaging (e.g. x-rays, MRI), and medical history review will be performed. Based on your diagnosis, treatment recommendations can be tailored to your specific condition and needs.
Failure to identify the cause of your pain can exacerbate the problem and/or delay proper medical care, ultimately leading to a longer road to recovery.
Osteoporosis Prevention
 How to prevent Osteoporosis & its progression:
How to prevent Osteoporosis & its progression:
- Proper Nutrition: A well-balanced diet rich in calcium and vitamin D is essential for bone health. Calcium strengthens bones, while vitamin D aids in calcium absorption. If needed, consult with a healthcare professional to determine if calcium and vitamin D supplements are necessary.
- Regular Weight-Bearing Exercise: Weight-bearing exercises help stimulate bone growth and increase bone density. Activities such as walking, jogging, dancing, and aerobics are beneficial for strengthening the bones in the foot and ankle. Engaging in these exercises for at least 30 minutes a day, several times a week, can yield positive results. Weight lifting or strength training also help stimulate bone growth and increase bone density, reducing the risk of fractures associated with osteoporosis.
- Fall Prevention: Preventing falls is crucial for individuals with osteoporosis. Wearing appropriate footwear with good traction and support is important for stability.
- Lifestyle Modifications: Avoid smoking and excessive alcohol consumption, as these habits can impair bone health. Smoking has been linked to decreased bone density, while excessive alcohol intake can interfere with calcium absorption. Maintaining a healthy weight and minimizing stress on the feet and ankles through proper body mechanics, posture, and supportive shoe wear can also be beneficial.
- Consultation with a Healthcare Professional: Regular check-ups and consultations with a healthcare professional are essential for early detection, diagnosis, and management of osteoporosis. We can provide personalized guidance on preventive measures and recommend appropriate screenings and treatments.
By adopting a proactive lifestyle that includes exercise and healthy habits, you can optimize bone health and reduce risk of osteoporosis-related complications.
Combat sweaty feet this summer!
 Excess moisture in shoes can hinder performance, cause discomfort, and increase risk of blisters and fungal/ bacterial infections of the skin and nails. Here are some expert recommendations on how to keep your foot-sweat under control:
Excess moisture in shoes can hinder performance, cause discomfort, and increase risk of blisters and fungal/ bacterial infections of the skin and nails. Here are some expert recommendations on how to keep your foot-sweat under control:
- Choose the right shoes. Shoes made from leather, suede, nubuck, canvas, and other natural materials are breathable, allowing for air circulation and prevention of excessive sweating . If these materials aren't an option, look for synthetic fabrics with breathable technologies like mesh.
- Rotate your shoes. Avoid wearing the same shoes every day to allow them to dry completely between wears. To help shoes dry faster, put them in direct sunlight fora few hours and add dryer sheets between wears. You can also add baking soda inside the shoes (if getting white residue on socks/feet won't bother you).
- Moisture-wicking socks. Wearing the proper socks for your sport or activity can make a huge difference in comfort-level and dryness. Socks made of materials such as polyester, nylon, and wool wick away moisture and are best for keeping feet cool, dry, and comfortable. (Cotton socks tend to trap moisture and keep socks damp.)
- Good hygiene. Wash your feet daily with anti-bacterial soap (like Dial), rinse well, and be sure to dry them completely, especially between your toes.
- Powder to the rescue. If you've done all the above and still have excessive moisture, add powder to the mix. Look for products with baking soda, zinc oxide, arrowroot, or kaolin clay for moisture absorption.
If you have specific concerns or conditions, consult with a healthcare professional for personalized recommendations.
Check your Soles: What to know about Flatfeet
 Flat feet can be inherited or develop over time with age, sports injuries, certain medical conditions, ligament/tendon damage or degeneration, increased weight, pregnancy, or from compensation due to inadequate support.
Flat feet can be inherited or develop over time with age, sports injuries, certain medical conditions, ligament/tendon damage or degeneration, increased weight, pregnancy, or from compensation due to inadequate support.
Flatfeet are seen in both children and adults and may be asymptomatic or symptomatic. For asymptomatic cases (especially in children), it's important to keep prevention in mind:
1. Eat healthy and stay hydrated to keep your cells functioning properly and help your body repair damage
2. Keep your muscles strong by exercising regularly, paying particular attention to ankle strengthening exercises
3. Wear supportive shoes when you're active
Flatfoot deformity can be progressive and may become symptomatic over time. Common complaints include achy, tired feet, or foot cramping after long periods of standing. Bunions, hammertoes, and arch collapse may also contribute, adding to the "flat" appearance of the feet.
If you have symptomatic flatfeet, the first step is to determine the cause. A proper evaluation with x-rays can answer questions and help direct a treatment plan. Every flatfoot is different! Treatment should be personalized and depend on your specific diagnosis.
For example, if the cause is:
- Tight muscles causing stress, destabilizing joints in the foot, a proper exercise program with an orthotic may be needed.
- Tendon degeneration, advanced imaging (MRI) may be needed to evaluate the extent of damaged tissue and assessing need for repair.
- Coalition of two bones, short-term immobilization in a boot or bracing may be recommended before jumping to surgery.
- Abnormal joint motion leading to arch collapse and instability, custom orthotics may be best for motion control and support.
-Chronic bone malalignment with abnormal joint wear and cartilage loss, bracing or surgery may become options.
Flatfeet aren't as simple as they seem. Your diagnosis might be more complex than a neighbor or even a family member! Custom orthotics are often the best non-surgical solution to help control abnormal motion in your feet, alleviating painful symptoms associated with flatfeet.
Prevention IS the best medicine! Schedule a consultation with us to help prevent worsening of symptoms.
Recognizing Signs of Diabetes in the Foot
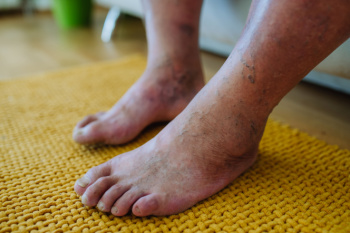
Diabetes can manifest in the feet through several noticeable signs. One common symptom is persistent numbness or tingling, often caused by nerve damage, known as diabetic neuropathy. This condition can lead to a loss of sensation, making it difficult to detect injuries or infections. Another sign is slow-healing sores or ulcers, which can develop from minor cuts or blisters due to poor circulation. Discoloration of the skin, such as redness, can indicate inflammation or infection. Swelling in the feet and ankles might also be present, signaling potential underlying issues. Additionally, changes in skin texture, including dryness or cracking, can occur. Fungal infections, particularly between the toes, are more frequent in diabetics. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can help you manage this serious condition.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact one of our podiatrists from Carolina Foot & Ankle. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact one of our offices located in Huntersville Office | 16419 Northcross Dr Suite A, Huntersville, NC 28078; Mooresvillle Office | 206 Joe Knox Avenue Suite D, Mooresville, NC 28117; and Mountain Island | 10310 Couloak Drive Suite 200, Charlotte, NC 28216 . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
